Doctors saved a baby in the womb from a deadly genetic disorder after successfully performing a unique brain surgery in utero, marking a significant milestone in fetal medicine.
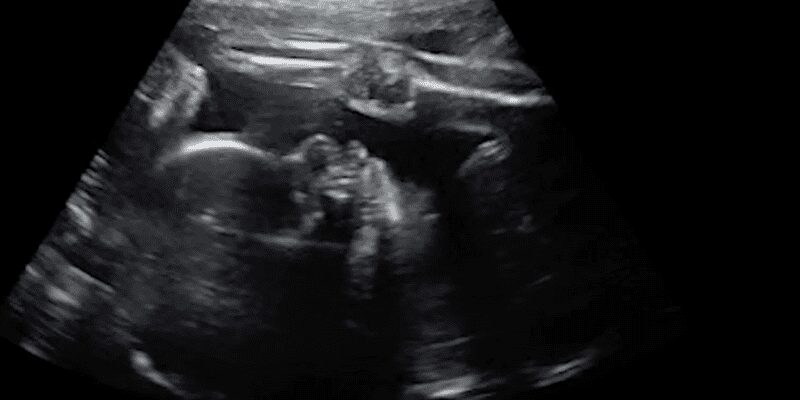
The story revolves around Derek and Kenyatta Coleman, a couple from Baton Rouge, Louisiana, who were thrilled to discover that they were expecting a child. Initial tests and screenings indicated a healthy pregnancy, and the couple was eagerly anticipating the arrival of their baby. However, during a routine 30-week ultrasound, they received devastating news – something was amiss with their baby’s brain, and her heart appeared enlarged.
Further investigation revealed that the baby was suffering from a rare condition called vein of Galen malformation (VOGM). This condition is characterized by an abnormality in the blood vessels within the brain, where arteries connect directly to veins instead of capillaries. This disrupts the normal blood flow, causing high-pressure blood to rush into the brain. VOGM can lead to a range of complications, including congestive heart failure, pulmonary hypertension, brain injury, and hydrocephalus.
According to Boston Children’s Hospital, studies have shown that approximately one-third of newborns with VOGM do not survive, while another third experience severe neurocognitive impairments despite treatment. Only one-third of affected individuals reach adulthood without significant compromise.
In the face of this daunting diagnosis, the Colemans decided to participate in a clinical trial that offered a glimmer of hope. Despite the potential risks, including preterm labor and brain hemorrhage for the baby, they believed it was their best chance to save their child.
A team of skilled medical professionals at Boston Children’s Hospital and Massachusetts General Hospital embarked on an unprecedented journey. At 34 weeks and 2 days’ gestational age, they performed a delicate surgery on preborn baby Denver Coleman. The procedure involved making incisions in the mother’s womb, accessing the baby’s skull, and operating on the developing brain. Throughout the surgery, ultrasound technology guided the medical team, enabling them to navigate with precision.
The successful surgery, conducted under such intricate circumstances, was documented in a case study published in an American Heart Association journal. Two days after the operation, Denver was born, weighing a relatively light 4.2 pounds. Although this weight is below the average range, Denver exhibited no birth defects and experienced minimal complications.
“I heard her cry for the first time and that just, I – I can’t even put into words how I felt at that moment,” Kenyatta told CNN. “It was just, you know, the most beautiful moment being able to hold her, gaze up on her and then hear her cry.”
“I gave her a kiss and she was just making little baby noises and stuff,” Derek said. “That was all I needed right there.”
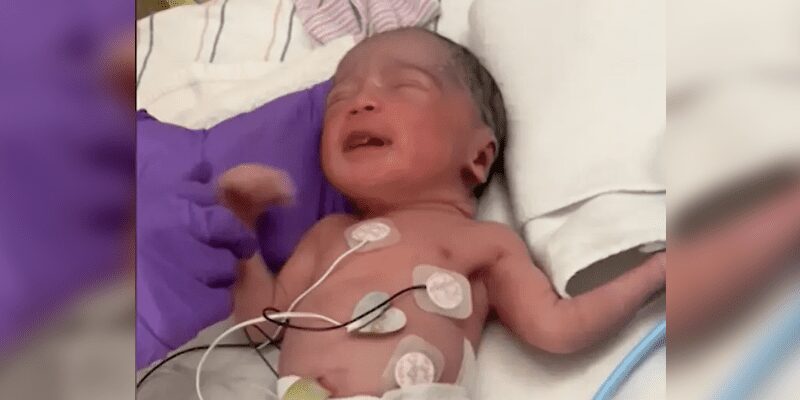
As Denver continued to grow, subsequent MRI scans revealed no signs of abnormal blood flow, and she required no cardiovascular assistance.
“We are pleased to report that at six weeks, the infant is progressing remarkably well, on no medications, eating normally, gaining weight and is back home. There are no signs of any negative effects on the brain,” remarked lead study author Darren B. Orbach, MD, PhD, co-director of the Cerebrovascular Surgery & Interventions Center at Boston Children’s Hospital and an associate professor of radiology at Harvard Medical School.
Currently, researchers and the Food and Drug Administration are collaborating to conduct trials aimed at evaluating the safety and effectiveness of this groundbreaking surgery. The medical community hopes that the results of these trials will pave the way for broader application, benefiting more families facing similar challenges.
Dr. Gary M. Satou, director of pediatric echocardiography at UCLA Mattel Children’s Hospital, emphasized the importance of collecting comprehensive data through the ongoing clinical trial to ensure positive outcomes in both neurological and cardiovascular health. By addressing vein of Galen malformation before birth, the medical community aims to prevent heart failure, reducing the risk of long-term brain damage, disability, and mortality in infants.
The successful brain surgery performed on Denver Coleman represents a significant milestone in fetal medicine. It showcases the potential of repairing malformations in the womb and gives a different path to parents who may be pressured to abort in such circumstances.
While this case is just the beginning, the medical community remains committed to furthering their research to ensure the safety and efficacy of this procedure. With continued advancements, they hope to provide more families with renewed hope and the possibility of brighter futures for their unborn children.



